PREGNANCY had been a breeze for Megan Batchelor.
She had not even had any morning sickness and had been able to carry on training and working as a personal trainer.
And after a tough labour, little Robyn looked like the perfect baby.
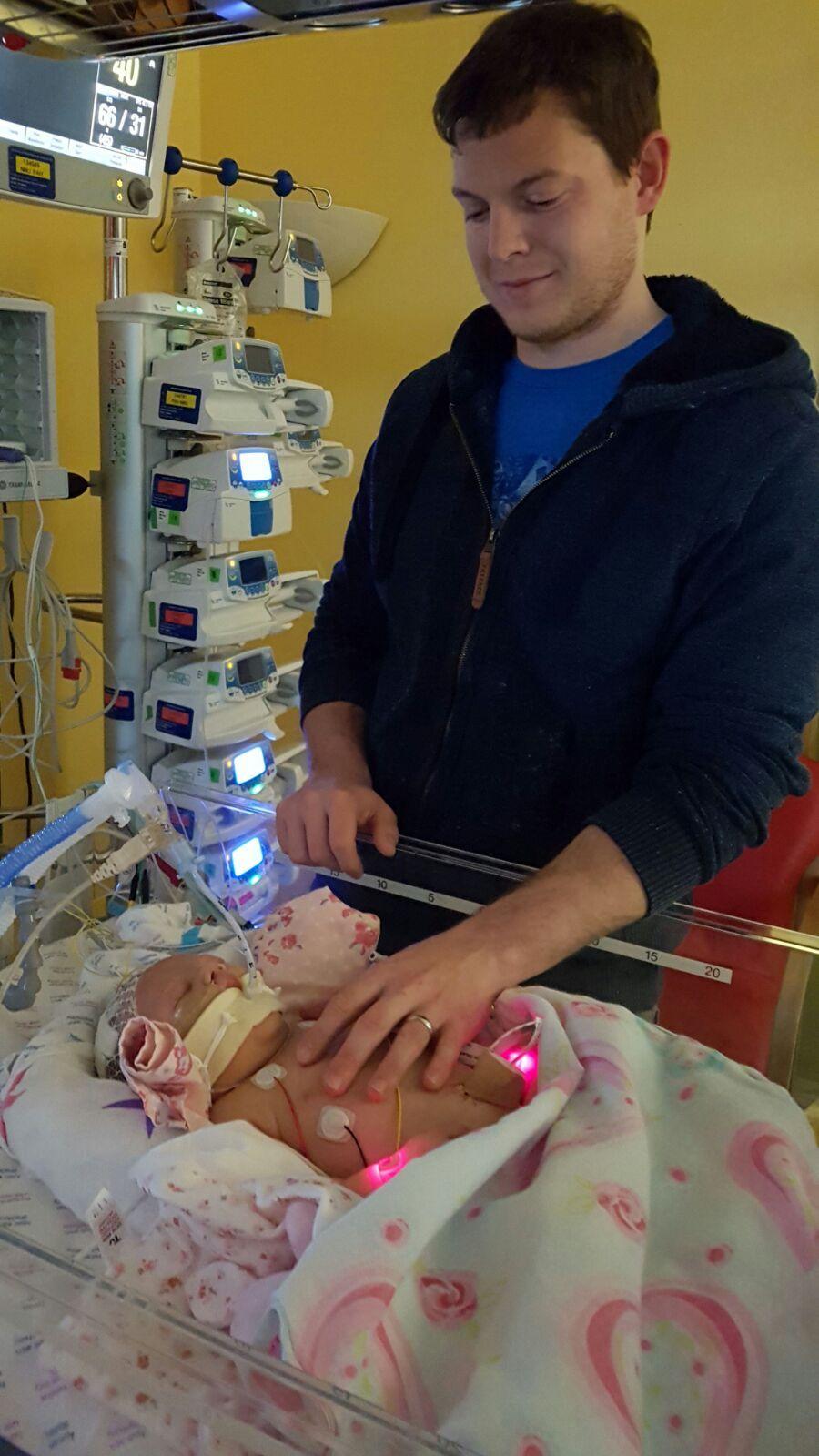
As Megan and her husband Mark cradled their tiny, beautiful girl, they could never have guessed that a few hours later she would be in intensive care, with her life hanging on a knife edge.
They were still in the labour suite on the afternoon of Robyn's birth, enjoying their first few hours of getting to know their new baby when a midwife noticed that something might not be quite right.
"She asked how long she'd been making these noises. They call it grunting – it's laboured breathing. She said she needed to go down to the neonatal unit to be checked up," says Megan.
"The next time I saw her was at 10pm. She was in a little ball on her front and was really struggling to breathe. It was so sad to see her."
Doctors didn't know at that point what was wrong with tiny Robyn and were treating her with broad spectrum antibiotics, while they waited for the results of blood cultures to come back.
Megan, 28, from Bitterne Park, says that although she was very upset, she didn't realise at the time just how sick Robyn was.
Now she struggles to speak when she remembers how, having gone to sleep on a ward, she was woken up in the night and told that she needed to get her husband back to the hospital and go to her daughter's bedside. She realises that doctors didn't know if her daughter was going to survive until morning.
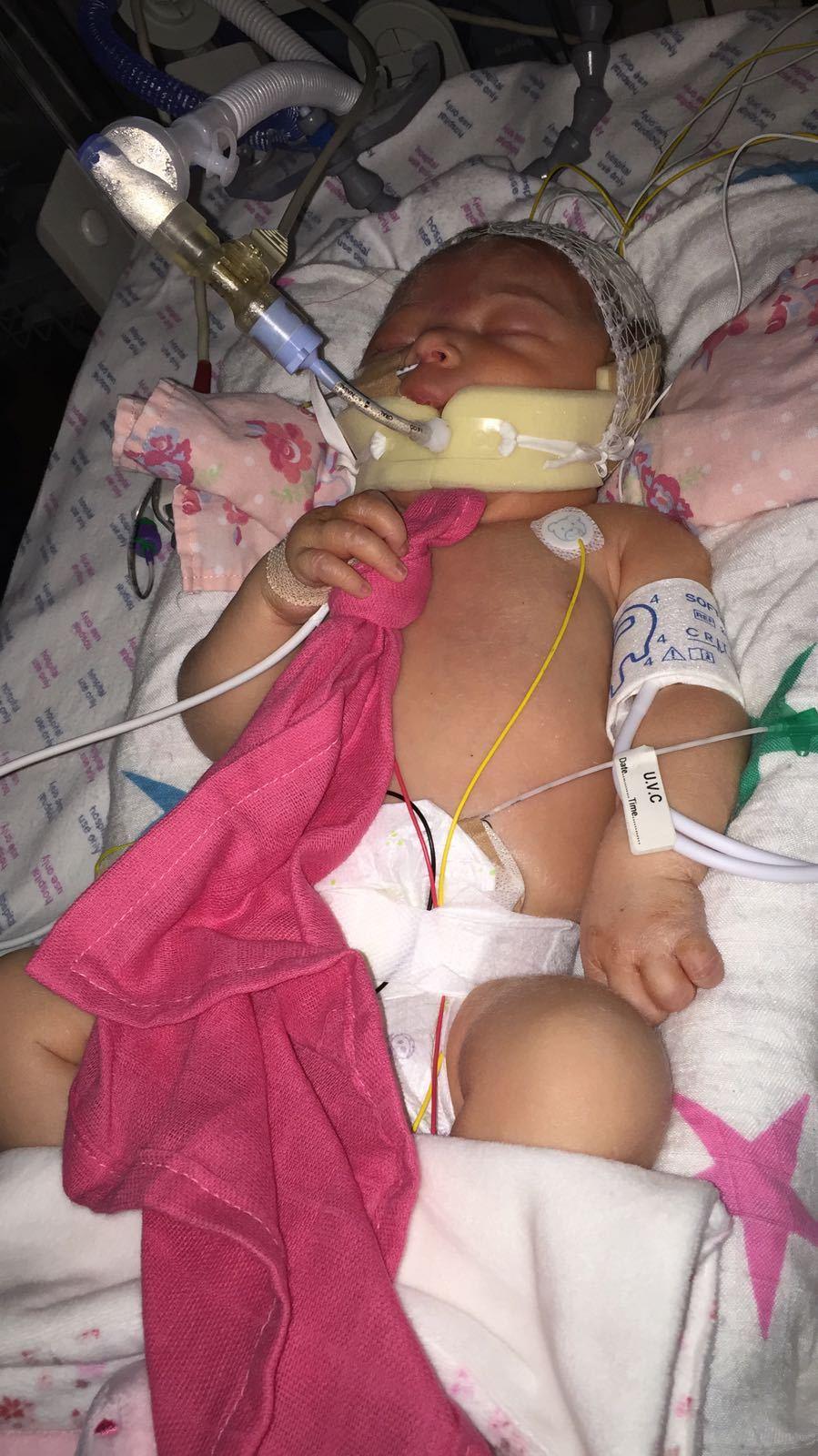
"She was fully sedated and on a ventilator," she says.
"There were lots of cables and netting on her head to monitor her brain activity, as she was having seizures.
"They were very good at not alarming me," she says.
"For the first 24 to 48 hours it was touch and go, but I only realised that looking back.
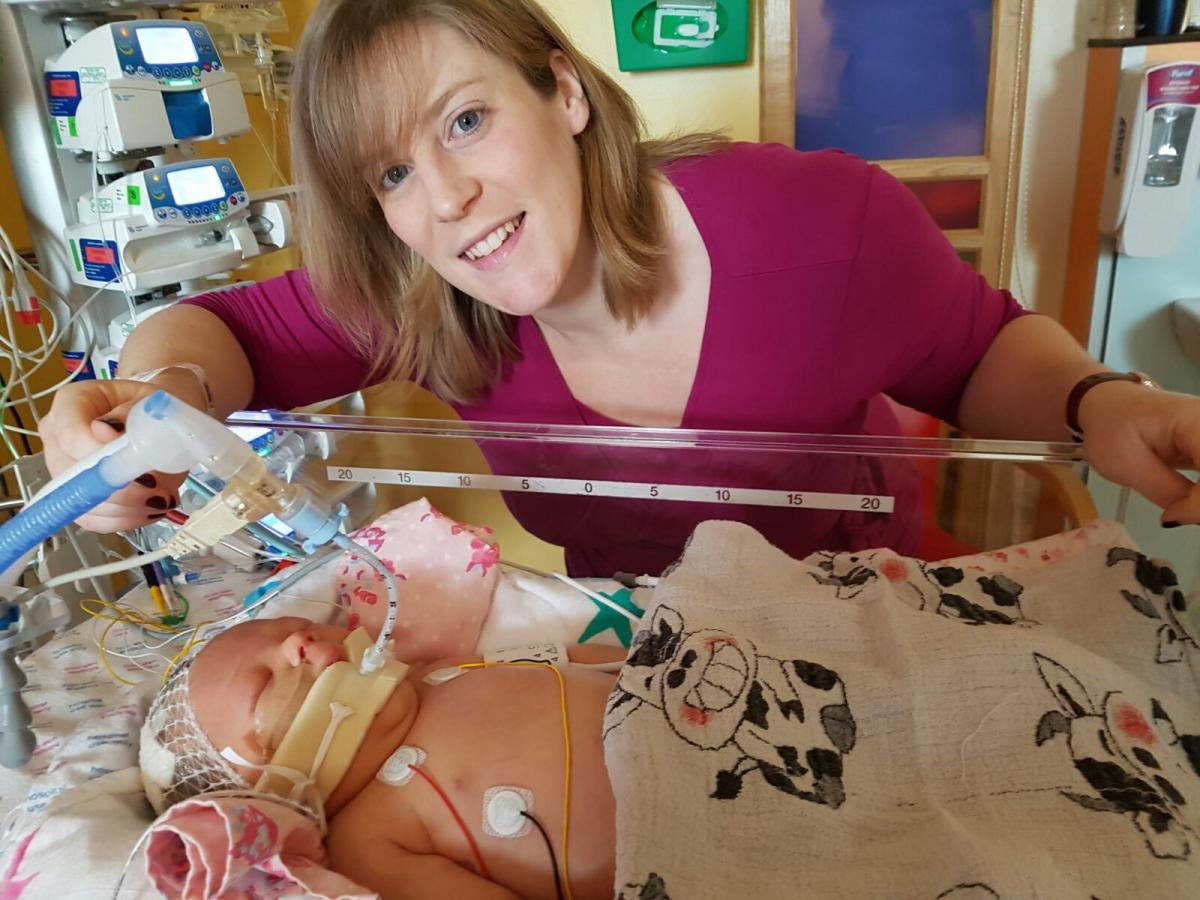
"I cried a lot at her bedside," she adds.
"It was really tough. As a new mother, you expect to struggle, but for completely different reasons. It was hard. I was left without a job a bit.
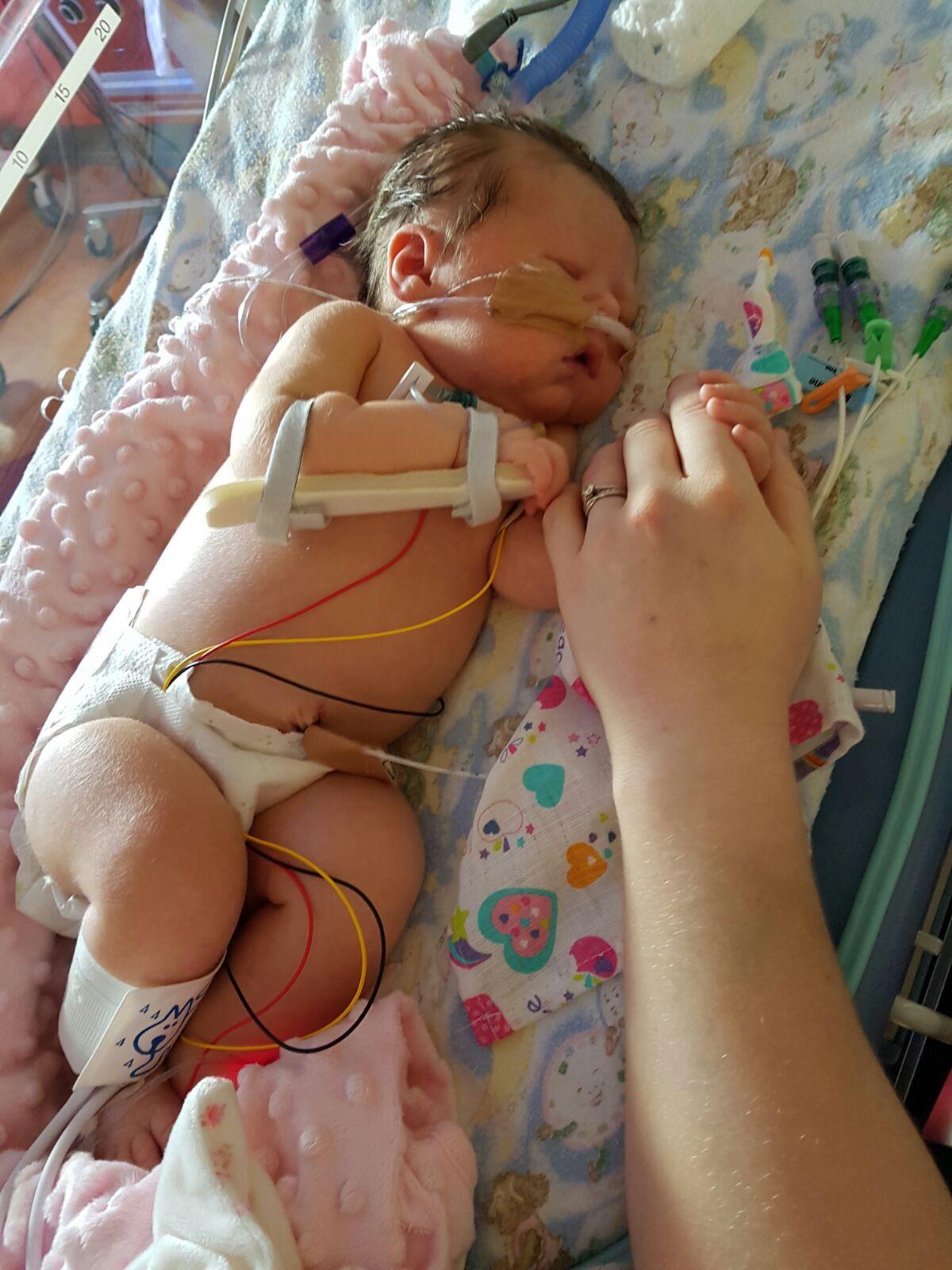
"I didn't even really get to hold her for the first week because she had so many lines in her.
"I couldn't believe it was happening. She had gone from completely normal to critically ill in such a short time."
Eventually, tests revealed that Robyn had a group B strep (GBS) infection and meningitis.
GBS is one of many bacteria that can be present in our bodies and doesn't usually cause any harm. It's estimated about one pregnant woman in five in the UK carries GBS in their digestive system or vagina.
Around the time of labour and birth, many babies come into contact with GBS and are colonised by the bacteria, and a small number become infected.
If a baby develops GBS infection less than seven days after birth, it's known as early-onset GBS infection. Most babies who become infected develop symptoms within 12 hours of birth. Symptoms include: being floppy and unresponsive, not feeding well, grunting, high or low temperature, fast or slow heart rates, fast or slow breathing rates and irritability.
One in ten babies born with GBS will die from the infection. Another one in five babies who survive the infection will be affected permanently. Early-onset GBS infection can cause problems such as cerebral palsy, deafness, blindness, and serious learning difficulties.
"We found that she had a group b strep infection that had been transferred from me," says Megan.
"There was an element of 'I gave this to her'. That was really hard to take.
"I don't think I'll ever get over the sense that it was my fault."
Robyn was in intensive care for ten days, before being transferred to a high dependency unit for four further days.
"Very gradually, she started to take back control of things that were being for her by machines. I was sitting by her and I was so excited when I saw her eyelids begin to flutter as the sedation wore off," remembers Megan.
After four further days, Robyn was allowed home, only to be rushed back to hospital when a scan revealed a large blood clot on her brain, which may have been a result of the infection. Megan and Mark were taught how to administer blood thinners and she has now finished the course of treatment.
Now, Robyn is a happy, healthy six month old who, thankfully, is showing no sign of long term effects of her illness.
But Megan is all too aware that without the fantastic care she received at the Princess Anne Hospital, Robyn might not have survived, or could have suffered serious long term consequences.
For this reason, as well as championing the NHS, Megan is keen to encourage other women to talk to their midwives about GBS.
"The information about group B strep is confusing. I want people to know about it and discuss it with their midwife so that they can make an informed decision.
"You can get a swab test done privately – it only costs £30 to £40 and you can do it yourself. I understand that the bacteria can be transient, so it might not be there when a test is done, but I think that it's really important that it's being discussed."
Current UK guidelines recommend a ‘risk factor’ approach to determine which women should be offered antibiotics in labour to prevent group B strep (GBS) infection in newborn babies. However, up to 40 per cent of newborn babies with GBS infection have no risk factors, apart from their mother unknowingly carrying GBS.
Testing is the only way to know if you are carrying GBS. If you are, steps can be taken to minimise the risk of your newborn baby developing GBS infection. Routine screening of all pregnant women for GBS carriage is not currently recommended by the UK National Screening Committee.
However tests can be done privately.
"There are things that are talked about and tested for when you're pregnant, like Down Syndrome. Considering the incidents of group B strep and how serious its consequences can be, with death and disability, I don't understand why is isn't discussed as standard. It seems too common not to be addressed.
"I know there is the question of the cost to the NHS of automatic testing, but I've been told that having Robyn in a high dependency unit would have cost the NHS £6,000 a day, so just the ten days that she was in there would have cost £60,000, before you start thinking about everything else. Imagine how many tests that could have paid for."
Now, Megan and Mark are trying to put the trauma of Robyn's first weeks behind them, and concentrate on being a family.
"We have regular developmental checks, and she's showing no sign of any long term effects, so we're very lucky," says Megan.
"It hasn't affected our intention to have more children. Some people seem surprised by that but there's no reason for it. If they had known, they would have given me antibiotics.
"I don't know if I'm more protective of Robyn than I would have been or not. But you do hold her a bit tighter when you remember that she nearly didn't survive."
For more information, visit the Group B Strep Support website: www.gbss.org.uk









Comments: Our rules
We want our comments to be a lively and valuable part of our community - a place where readers can debate and engage with the most important local issues. The ability to comment on our stories is a privilege, not a right, however, and that privilege may be withdrawn if it is abused or misused.
Please report any comments that break our rules.
Read the rules hereLast Updated:
Report this comment Cancel