NHS waiting lists in England have fallen for the fourth consecutive month, according to new figures, although the number of people waiting longer than 18 months for treatment has increased.
Cancer waiting times also remain well below target, the data shows, with charities calling for a long-term cancer strategy.
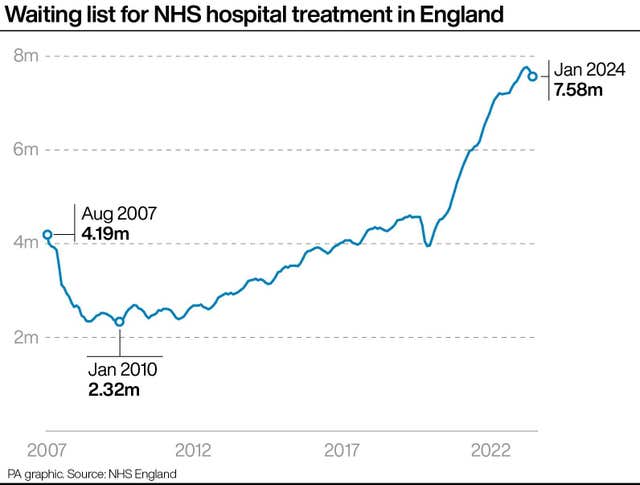
An estimated 7.58 million treatments relating to 6.32 million patients were waiting to be carried out at the end of January, down slightly from 7.60 million treatments at the end of December.
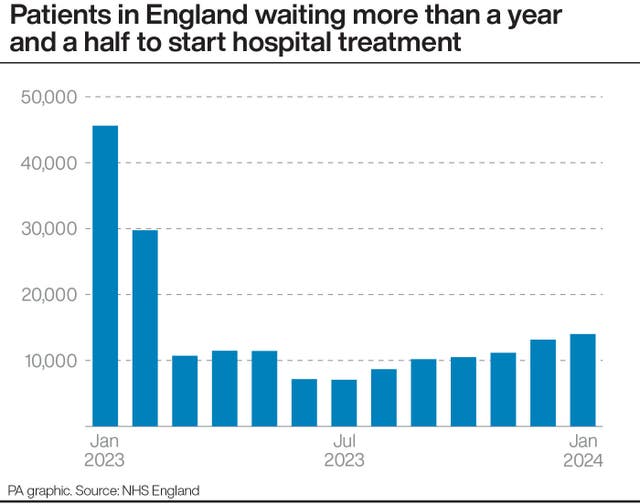
However, the number of people waiting more than 18 months went up to 14,013 from 13,164 at the end of December.
The Government and NHS England set the ambition of eliminating all waits of more than 18 months by April 2023, excluding exceptionally complex cases or patients who choose to wait longer.
Those waiting more than 52 weeks to start treatment fell to 321,394 from 337,450 in December, with an ambition to eliminate all waits of more than a year by March 2025.
Ministers have blamed waiting lists on ongoing industrial action in the NHS.
The new figures come after junior doctors in England walked out on the longest strike in the history of the health service – six days – at the start of the year.
Health Secretary Victoria Atkins said the Government’s “commitment to cutting waiting times is unwavering”.
She added: “This has been achieved despite disruptive strikes and record winter pressures on our NHS services.”
Elsewhere, some 70.9% of patients urgently referred for suspected cancer in January were diagnosed or had cancer ruled out within 28 days, down from 74.2% the previous month and below the target of 75%.
GPs in England made 249,787 urgent cancer referrals during the month, up from 219,841 in December and also up year-on-year from 228,402 in January 2023.
The proportion of patients in England waiting longer than 62 days in January from an urgent suspected cancer referral or consultant upgrade to their first definitive treatment for cancer was 62.3%, down from 65.9% in December and below the target of 85%.
Minesh Patel, head of policy at Macmillan Cancer Support, said “this can’t go on”.
“Healthcare professionals are doing all they can but are working in a permanent state of crisis,” he added.
“If the UK Government acts now, we can turn this around and ensure our cancer system is fit for purpose in the years to come.
“We need a long-term cancer strategy in England that provides the investment and focus needed so that everybody with a cancer diagnosis gets the timely and quality care they deserve.”
Professor Pat Price, who co-founded the #CatchUpWithCancer campaign, described the situation as “a disaster for cancer patients” and called for “a radical new cancer plan and a clear implementation plan to improve waiting times and cancer survival”.
Responding to the figures, shadow health secretary Wes Streeting said: “The Conservatives have broken every pledge they made on getting NHS waits down.
“They were meant to have eliminated the longest waits of 18 months or two years, but under Rishi Sunak more and more patients face years of their lives being put on hold.”
Sarah Woolnough, chief executive of think tank The King’s Fund, said: “Five years ago, these numbers would have been difficult to comprehend.
“The narrative of NHS performance has become acclimatised to the extraordinary. We used to comment about 18-week waits for routine care rather than 65 weeks, or talk about winter pressures rather than year-round crises.”
In February, the number of people waiting more than 12 hours in A&E departments in England from a decision to admit to actually being admitted was 44,417, down from 54,308 in January, which was the second highest figure on record.
The number waiting at least four hours from the decision to admit to admission has also fallen, from 158,721 in January to 139,458 last month.
Some 70.9% of patients in England were seen within four hours in A&Es, up slightly from 70.3% in January.
The NHS recovery plan sets a target of March 2024 for 76% of patients attending A&E to be admitted, transferred or discharged within four hours.
Ms Woolnough added that “it is unlikely” that these “watered down” targets will not be met.
“The Government set interim targets such as 76% of people being seen within four hours in A&E, compared with the NHS standard of 95%,” she added.
“Ministers also set the expectation that no heart attack or stroke patients would wait more than 30 minutes for an ambulance, far longer than the NHS standard of 18 minutes. Even with these lower goals, both these targets are unlikely to be met by the end of the month.”
Professor Sir Stephen Powis, NHS national medical director, said “demand for NHS services across the country remains high”.
He said: “It is testament to the hard work of staff and the measures in our elective recovery plan that despite the longest period of industrial action in NHS history in January, with one in five days affected, staff still managed to bring the waiting list down – staff delivered more activity than before the pandemic using a range of innovative and new technologies to ensure we continue to make progress on the longest waits for our patients.”
Louise Ansari, chief executive at Healthwatch England, said: “Accessing urgent and emergency care is a real priority for patients.
“Long waits in A&E are particularly frustrating for people and put lives at risk.
“We therefore welcome the modest improvements on patients admitted, discharged or transferred within four hours and those waiting more than 12 hours.
“However, we know that measuring progress against these targets alone won’t improve patient experience.
“Our evidence shows that there are other factors that matter to patients, such as how quickly they are initially triaged, their access to food, water, and pain relief, and the quality of communication while waiting for care.”




Comments: Our rules
We want our comments to be a lively and valuable part of our community - a place where readers can debate and engage with the most important local issues. The ability to comment on our stories is a privilege, not a right, however, and that privilege may be withdrawn if it is abused or misused.
Please report any comments that break our rules.
Read the rules here